A Survey of the Standard Radiation Protection Practice in Radiography Departments of Some-Selected Tertiary Hospitals in South East Nigeria
DOI:
https://doi.org/10.59667/sjoranm.v25i1.14Keywords:
Radiation, Protection, Nigeria, RadiographersAbstract
Background
The radiation protection practices implemented in the radiology departments of tertiary hospitals in southeastern Nigeria have a significant impact on the safety of patients, healthcare professionals, and the general public. However, there is a lack of comprehensive understanding regarding adherence to standard radiation protection protocols in these departments.
Objectives
This study aimed to assess the standard radiation protection practices implemented in radiography departments within selected tertiary hospitals in Southeast Nigeria.
Methods
The study was a prospective cross-sectional survey. These hospitals include the University of Nigeria Teaching Hospital, Ituku Ozalla (UNTH), National Orthopedic Hospital Enugu (NOHE), Nnamdi Azikiwe Teaching Hospital, Nnewi, and Federal Medical Center Abakaliki. A total of 72 radiographers working in the abovementioned hospitals were included in the study.
Results
The quantitative findings revealed varying degrees of compliance with standard radiation practices. While all the hospitals employed appreciable shielding measures and demonstrated knowledge of radiation safety guidelines, the quality control measures and personnel/workplace monitoring were drastically low. The research also showed that little or no work has been done by hospital management and radiographers in updating their existing knowledge, as it pertains to standard radiation protection measures.
Conclusions
This research thus highlights the urgency of standardized radiation protection practices within radiography departments. Recommendations include the allocation of adequate resources to ensure the availability of essential protective equipment and infrastructure and the development of comprehensive formal training programs for radiographers and other healthcare personnel involved in radiological procedures.
----------------------------------------------------------------------------------------------------------------------------------------
A SURVEY of the STANDARD RADIATION PROTECTION PRACTICE in RADIOGRAPHY DEPARTMENTS of SOME-SELECTED TERTIARY HOSPITALS in SOUTH EAST NIGERIA
Ezenwaka, Augusta Amarachi*1,ORCID; Ibe, Chijioke K.1; Ezugwu, Wisdom K.1; Ifeanyi, ThankGod O.1; Nwadike, Uchechukwu I.1
Swiss Journal of Radiology and Nuclear Medicine - www.sjoranm.com - Rosenweg 3 in CH-6340 Baar, Switzerland
Introduction
1. Background of the study
The increasing use of diagnostic radiology is unquestionably beneficial. However, per capita exposure to medical radiation has increased in the last two decades and appears to be still increasing (1, 2). Several studies carried out in Nigeria have shown that the level of adherence to and usage of radiation protection practices and devices is very low, resulting in unnecessarily high levels of ionizing radiation exposure for patients and healthcare workers (3, 4). Thus, the issue of medical radiation protection and its importance for the health of both patients and radiation professionals has gained increasing interest (5, 6). It is already well established that the effects of radiation are cumulative and lead to an increased incidence of cancer, cell death, genetic damage, and numerous forms of body tissue pathology; hence, ionizing radiation at any quantity is potentially detrimental to health (7, 8). Radiation damage can occur in many ways, inclu-ding skin erythema, hair loss, vascular damage, internal bleeding, cataracts, cancers, weakened immune systems, sterility, mutations in offspring, premature aging, and death. (3)
During radiologic examinations, several factors are controlled by radiographers, which can maximize the diagnostic value of the image and minimize patient exposure (9, 10). Applying the principles of radiation protection can prevent the deterministic effects of ionizing radiation and decrease the related stochastic effects (11). Although several protective measures are considered significantly simple, radiographers’ proper observance of these measures eliminates most of the unwanted and unnecessary radiation hazards. The fundamental principles of radiation protection are justification, optimization, and dose limits (12, 13). These fundamental principles imply that only individuals who derive maximum benefits from such exposure to ionizing radiation are exposed (Justification); radiation dose as a result of medical exposure is enough only to achieve the needed diagnosis (Optimization); and the dose should also be set to ensure that no individual faces an unacceptable risk in normal circumstances (dose limit) (14, 15).
Moreover, the use of lead aprons and protective equipment for patients and their companions when the presence of companions during radiographic examination is necessary is highly impor-tant (16, 17). Consequently, the availability and use of radiation protection measures, such as time, distance, protective shields (lead shielding devices), personnel dosimeters, and sound know-ledge of radiation protection, are essential (18, 19). To ensure the safety of patients, providers, and staff members, the healthcare community must become familiar with the terminology, common equipment, and standard practices used in radiation safety and monitoring. This has led to the urgent need for the radiology departments of tertiary hospitals in southeast Nigeria to abide by standard radiation protection practices for quality and efficient healthcare delivery.
Yusuf et al. (20), in Damaturu, Yobe state, shed light on significant gaps in radiation protection measures among medical personnel. While certain protective equipment, such as lead aprons and shields, is accessible, this study reveals concerns about shortages of thyroid shields and, at times, lead gloves, heightening the risk of thyroid cancer. The absence of adequate monitoring devices leaves workers vulnerable to potential radiation overexposure. This research under-scores the vital necessity of complete safety compliance, urging the thorough implementation of quality assurance initiatives, consistent professional development programmes, and the incorporation of monitoring devices to ensure comprehensive protection. By addressing these issues, the study emphasizes the potential to minimize repeat exposures, enhance radiograph quality, and ultimately safeguard both patients and medical staff.
The study conducted by Eze et al. (3) focused on radiation protection practices among Radiographers in Lagos, Nigeria. Radiographers generally had a good understanding of radiation protection, scoring an average of 73% in knowledge assessment, outperforming a similar study in England. However, the use of exposure charts was deemed crucial, especially in centers lacking modern equipment, to prevent unnecessary patient irradiation. The presence of obsolete X-ray machines without quality assurance tests and the absence of medical physicists raised concerns.
Protective measures such as gonad shields were often ignored in government hospitals, possibly due to lax regulatory oversight. Discrepancies in radiation protection devices were observed between radiographers' claims and actual availability in government hospitals. The importance of wearing dosimeters was highlighted to avoid exceeding radiation dose limits.
In the Association of Radiographers of Nigeria's journal, Skam et al. (21) examined radiographic room design and radiation protection in diagnostic facilities in Katsina State, Nigeria. The study showed that X-ray rooms in the surveyed centers lacked proper radiation protection for operators and others within the controlled area, potentially due to inadequate room dimensions. The authors highlighted the importance of the inverse square law, where radiation intensity decreases with distance from the source, emphasizing that larger room dimensions increase the distance between the X-ray tube and the control room, reducing radiation exposure. However, the diagnostic facilities did not adhere to the recommended guide-lines from the NNRA and IAEA in terms of room design.
A study conducted in Rwandan public hospitals by Patrick et al. (22) revealed similarities between Nigerian and Rwandan hospitals regarding personal radiation monitoring. The study highlighted the inadequate enforcement of personal radiation dosimeter use and reading, which poses potential risks of radiation exposure to staff. The monitoring frequency of the dosimeters was far from the recommended standards, with only 3% being monitored monthly and 34% every three months.
Al-sayyari et al. (23) carried out research in Saudi Arabia. Their research aimed to assess radiation protection practices among radiography students in Saudi Arabia. They carried out the study among 110 radiologic technologist students and discovered that all the students in the study made use of TLD cards. They also had good knowledge of the radiation protection practices that are necessary when taking radiographs.
Fiagbedzi et al. (24) surveyed radiographers in Ghana to assess their radiation protection practices and discovered that while more than ninety percent of the radiographers had personnel dosimeters, only 25% of the radiographers made use of the dosimeters; however, the adherence to radiation protection practices was fairly satisfactory and was higher among the 35-45 years age group. Additionally, they discovered that radiographers who had worked for less than 5 years had a higher odds ratio of having completed some radiation training course.
Abdelrahman et al. (25) carried out a survey among radiologists in tertiary hospitals in Jordan to determine their level of compliance with radiation protection practices. They discovered that among the 62 respondents in the study, the use of lead aprons and thyroid shields was commonplace, whereas the use of lead-lined eyeglasses was very rare (3.2%), 93.5% of the radiologists always used a personal dose monitoring device, and 66.1% of the radiologists reported unnecessary exposure to the patient.
Lewis et al. (26) carried out a qualitative study among South African radiographers to determine their adherence to radiation protection practices. The researchers found that most of the radiographers had good knowledge of radiation protection; however, compliance remained a personal choice, and some of the factors that made them less likely to carry out radiation protection included the rush to attend to emergency patients, patients’ knowledge of radiation protection, inadequate training during analog-to-digital migration, managerial support, imaging referrals, etc. The radiographers concluded that although the level of knowledge was high, the practice did not reflect the knowledge because the radiographers did not internalize the information that they had known properly; they proposed ways of improving compliance with radiation protection guidelines.
The radiation protection practices implemented in the radiology departments of tertiary hospitals in southeastern Nigeria have a significant impact on the safety of patients, healthcare professionals, and the general public. However, there is a lack of comprehensive understanding regarding adherence to standard radiation protection protocols in these departments (2). This research aimed to identify the current state of radiation protection practices in the radiography departments of several selected hospitals in south-eastern Nigeria and assess their compliance with established standards. Although studies have been conducted across different geopolitical zones with respect to these growing concerns, as of the time of this study, no concrete survey has been carried out across the radiology depart-ments of tertiary hospitals in southeastern Nigeria. Hence, this research seeks to bridge this gap.
2. Methods
A cross-sectional prospective study was conducted in four federal government-owned hospitals in southeastern Nigeria. These hospitals include the University of Nigeria Teaching Hospital, Ituku Ozalla (UNTH), National Orthopedic Hospital Enugu (NOHE), Nnamdi Azikiwe Tea-ching Hospital, Nnewi, and Federal Medical Center Abakaliki. A total of 72 radiographers working in the abovementioned hospitals were included in the study. The study was carried out between August 2023 and February 2024. The inclusion criteria included practicing radiographers in government-owned tertiary hospitals in south-eastern Nigeria and receiving a willingness to participate in the study.
2.1 Method of Data Collection
A well-structured questionnaire was used for the collection of the data. All participants were provided with clear information about the purpose of the study, and informed consent was obtained prior to their participation. The questionnaire comprises three sections. Section A is based on the sociodemographic information of the respondents. Section B was concerned with assessing the integrity of the shielding used and the X-ray room design in reducing radiation exposure; section C was concerned with evaluating the level of radiation protection knowledge and its application, which was exhibited by radiographers. Finally, section D assesses the effectiveness of workplace and personnel monitoring and quality control.
A total of 72 well-composed questionnaires were distributed to the sample for data collection. These were completed and returned, after which the information provided was extracted and analyzed. The questionnaire used for this study is provided in the Appendix.
2.2 Data Analysis
The data were analyzed using the Microsoft Statistical Package for Social Sciences (SPSS) version 25, and the Pearson correlation coefficients were calculated for the study parameters. The demographic data were analyzed using descriptive statistics. The data were analyzed using a quantitative method. The quantitative data collected were analyzed using tables for frequency and percentage.
3. Results
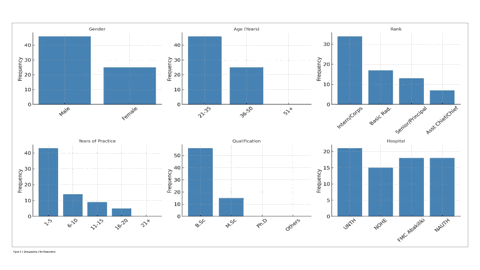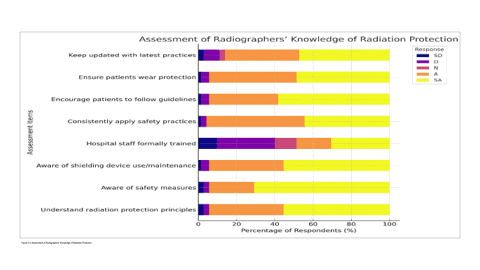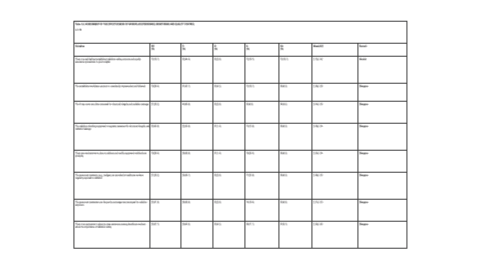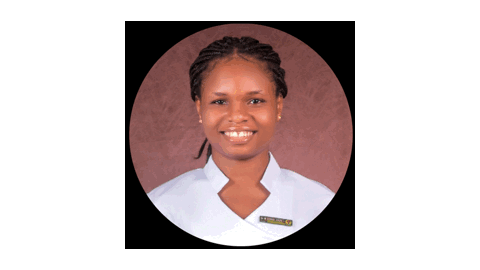
A cross-sectional study was carried out among practicing radiographers in several selected tertiary hospitals in southeastern Nigeria. A total of 72 questionnaires were administered to the respondents; the questionnaires were manually distributed and successfully completed and returned, for a response rate of 100%. The analysis in this research was performed using SPSS (Statistical Package for Social Sciences) version 25, where respondents’ answers were analyzed using both descriptive and inferential statistics and are presented in tables as follows Figure 3.1: Demographics of the Respondents.
As depicted in Figure 3.1 above, a total of 46 males (63.9%) and 25 females (34.7%) participated in the study. Forty-six respondents (63.9%) were within the age range of 21–35 years, and 25 respondents (34.7%) were within the age range of 36–50 years. Thirty-four respondents (47.2%) were interns/corps members, 17 respondents (23.6%) were basic-level radiographers, 13 respondents (18.1%) were senior/principal radiographers, and 7 respondents (9.7%) were assistant chief/chief radiographers. Forty-three respondents (59.7%) had practiced for 1–5 years, 14 respondents (19.4%) had practiced for 6–10 years, 9 respondents (12.5%) had practiced for 11–15 years, and 5 respondents (6.9%) had practiced for 16–20 years. Fifty-six respondents (77.8%) had a B.Sc, and 15 respondents (20.8%) had an M.Sc. Twenty-one respondents (29.2%) worked at the University of Nigeria Teaching Hospital (UNTH), 15 respondents (20.8%) worked at the National Orthopaedic Hospital Enugu (NOHE), 18 respondents (25.0%) worked at the Federal Medical Centre (FMC) Abakaliki, and 18 respondents (25.0%) worked at the Nnamdi Aziki-we University Teaching Hospital (NAUTH). The detailed data are shown in Table 3.1 (see Appendix).
As illustrated in Figure 3.2, the majority of the respondents affirmed (agree) that the X-ray room design is purpose-built for radiological procedures (91.7%), the lead-lined walls and doors in the X-ray room are in good condition (79.1%), the X-ray control room is adequately shielded to reduce radiation exposure to the operator (82.0 %), the availability of radiation shielding equipment (lead aprons, lead gloves, googles, gonads, and thyroid shields) is adequate (73.6%), the shielding devices (lead aprons, lead gloves, googles, gonads, and thyroid shields) are in good condition (68.0%), the calibration of the X-ray machine is accurate (61.3%), the X-ray machine is equipped with appropriate safety interlocks to prevent accidental exposure (68.1%), and the distance between the X-ray tube and erect bucky 180 cm from the focal spot (65.3%). However, the majority of the respondents were undecided as to whether the personnel dosimeters for radiographers were adequate and in good condition (mean value = 3.11± 1.37). The detailed data are shown in Table 3.2 (see Appendix).
As depicted in Figure 3.3, the majority of the respondents strongly agreed that they understood the principles of radiation protection and the regulatory guidelines and local protocols related to radiation safety (94.5%), were aware of the appropriate safety measures to minimize radiation exposure to patients and staff (94.4%), were aware of the proper use and maintenance of radiation shielding devices and equipment (94.5 %), consistently applied radiation safety practices during radiographic procedures (95.5%), and encouraged patients to follow radiation safety guidelines during their examinations (94.4%). Additionally, they were advised that patients wear appropriate protective devices during radiographic procedures (94.4%), and they kept themselves updated with the latest advancements in radiation protection practices (86.1%). However, the majority of the respondents were not sure if the healthcare workers in their hospital received formal training in radiation safety and protection (mean value = 3.29±1.43). The detailed data are shown in Table 3.3 (see Appendix).
As depicted in Table 3.4 (see Appendix), the majority of the respondents disagreed with the following: There are well-defined established radiation safety protocols and quality assurance procedures in your hospital (62.5%), the established workplace protocol is consistently implemented and followed (69.5%), the X-ray rooms are often assessed for structural integrity and radiation leakage (84.8%), the radiation shielding equipment is regularly assessed for structural integrity and radiation leakage (76.4%), there are mechanisms in place to address and rectify equipment malfunctions promptly (65.3%), the personnel dosimetry (e.g., badges) is provided to healthcare workers regularly exposed to radiation (65.3%), and the personnel dosimeters are frequently exchanged and analyzed for radiation exposure (70.8%). There is also a mechanism in place to raise awareness among healthcare workers about the importance of radiation safety (77.9%). However, regarding whether there are well-defined established radiation safety protocols and quality assurance procedures in your hospital, the majority of the respondents were not sure (mean value = 2.72±1.42).
Discussion
The findings of this study showed that while X-ray rooms are purposely built for radiological procedures with walls and control rooms adequately lead-lined to evert or reduce radiation exposure to people in adjacent rooms as well as to the operator (radiographer) in the cubicle, there is a slight lack of compliance in the area of personal radiation protective equipment (PPE). In the hospitals visited for this study, the lead aprons, gonads, and thyroid shields were fairly adequate. Additionally, approximately 70% of the radiographers did not have dosimeters, while those who had rarely worn them while on duty.
Furthermore, the results also showed that the radiographers in the hospitals included in the study possessed sound knowledge and applica-tion of radiation protection measures, as they related to regulatory guidelines, the use of shielding equipment, and patient orientation. However, there is no formal training on radiation safety and protection for radiographers or other healthcare workers. Additionally, radiographers rarely update themselves with the latest advancements in radiation protection practices. This only means that, outside the formal school walls, little or nothing is done by the hospital or the radiographers to improve their knowledge, as it pertains to radiation protection knowledge.
Again, the quality control measures and work-place/personnel monitoring in the hospitals used for this study were abysmally poor. First, there is no well-defined quality control procedure in hospitals. These findings show that diagnostic equipment such as X-ray machines, digitizers, and cassettes, among others, is not checked for functional integrity; thus, these devices are left to use until heavy and noticeable damage occurs before service engineers are consulted. This also means that personal radiation protective equipment (PPE), such as lead aprons, gonads, and thyroid shields, even the operator’s cubicle, are rarely assessed for structural integrity and replacement. Hence, no adequate radiation protection measures are put in place, and it puts the patients, radiographers or patient’s relatives in cases where it is required that they be present in the diagnostic room during radiological procedures.
Conclusion
In conclusion, this study revealed that in the area of optimal radiation protection practices among radiographers, there is much additional work to be done.
From the study above, it is evident that while most radiographers demonstrate an appreciable level of knowledge in radiation protection, there is a large gap in the application of this knowledge. Therefore, hospital management and radiology unit leadership must take action to address the situation, starting by implementing the recommendations outlined above.
Correspondence to:
https://orcid.org/0009-0004-6732-5990
Declarations
Consent for publication: The author clarifies that written informed consent was obtained and the anonymity of the patient was ensured. This study submitted to Swiss J. Rad. Nucl. Med. has been conducted in accordance with the Declaration of Helsinki and according to requirements of all ap-plicable local and international standards. All authors contributed to the conception and design of the manuscript, participated in drafting and revising the content critically for important intel-lectual input, and approved the final version for publication. Each author agrees to be accoun-table for all aspects of the work, ensuring its accuracy and integrity. Written informed consent was obtained from the patient's legal guardians for the publication of this case report and any accompanying images.
Competing interests: No competing interests.
Funding: No funding resources.
Ethical approval was obtained from the Health Research Ethics Committee of the University of Nigeria Teaching Hospital (UNTH/HRC/2025/02/3036). The approval covered the use of data collected between August 2023 and February 2024. Participation was voluntary, informed consent was obtained from all respondents, and confidentiality of the data was maintained throughout. All participants provided written informed consent before completing the questionnaire. Participation was voluntary, and responses were treated with confidentiality.
Conflict of interest:
The authors declare that there were no conflicts of interest within the meaning of the recommendations of the International Committee of Medical Journal Editors when the article was written.
Disclaimer/Publisher’s Note:
The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of Swiss J. Radiol. Nucl. Med. and/or the editor(s). Swiss J. Radiol. Nucl. Med. and/or the editor(s) disclaim responsibility for any injury to people or property resul-ting from any ideas, methods, instruc-tions or products referred to in the con-tent.
License Policy:
This work is licensed under a Creative Commons Attribution 4.0 International License.
This license requires that reusers give credit to the creator. It allows reusers to distribute, remix, adapt, and build upon the material in any medium or format, even for commercial purposes.
Check out our journal's LinkedIn profile with over 10 K registered followers from the Radiologic & Nuclear Medicine Imaging field: LinkedIn
References
- Madsen MT, Anderson JA, Halama JR, Kleck J, Simpkin DJ, Votaw JR, et al. AAPM Task Group 108: PET and PET/CT Shielding Requirements. Med Phys [Internet]. 2005 Dec 19;33(1):4–15. http://doi.wiley.com/10.1118/1.2135911
- Abdelrahman MA, Abu Alfwares A, Alewaidat H, Alhasan M, Rawashdeh MA, Al Mousa DS. Compliance With Radiation Protection Practices Among Radiologists. Health Phys [Internet]. 2018 Sep;115(3):338–343. https://doi.org/10.1097/hp.0000000000000886
- Eze C, Irurhe N, Njoku J, Olowu O, Abonyi L.
Assessment of radiation protection practices among radiographers in Lagos, Nigeria. Niger Med J [Internet]. 2013;54(6):386. https://doi.org/10.4103/0300-1652.126290 - IAEA. Justification and optimization | IAEA. [Internet]. 2011. https://www.iaea.org/resources/rpop/resources/international-safety-standards/justification-and-optimization
- Kim JH. Three principles for radiation safety: time, distance, and shielding. Korean J Pain [Inter-net]. 2018 Jul 31;31(3):145–6. http://www.epain.org/journal/view.html?doi=10.3344/kjp.2018.31.3.145
- ANSTO. What is radiation? [Internet]. 2023. https://www.ansto.gov.au/education/nuclear-facts/what-is-radiation
- Ahern M, McEntee MF, Moore N. Radiographers' atti-tudes toward the use of lead contact shiel-ding. J Med Imaging Radiat Sci. 2023 Sep; 54(3):415–420. https://www.jmirs.org/article/S1939-8654(23)01798-8/fulltext.
- Vañó E, Miller CJ, Rehani MM, Kang K, Rosenstein M, Ortiz-López P, et al. Annals of the ICRP [Internet]. Vol. 44, Protection, International Commission on Radiological. 2015. 1–143 p. www.icrp.org
- Cherry SR, Sorenson JA, Phelps ME. Radiation Safety and Health Physics. In: Physics in Nuclear Medicine [Internet]. Else-vier; 2012. p. 427–42. https://linkinghub.elsevier.com/retrieve/pii/B978141605198500023X
- Connor N. What is ALARA. Connor, Nick [Internet]. 2019;1. https://www.radiation-dosimetry.org/what-is-alara-definition/
- NNRA. Nigerian Radiation Safety in Diagnostic and Interventional Radiology Regulations, 2006. [Internet]. 2006;(19):661–92. https://nnra.gov.ng/nnra/page-diagnostic___interventional_radiology
- IAEA. Radiation Protection and Safety of Radiation Sources: International Basic Safety Standards. IAEA Safety Standards Series No. GSR Part 3. [Internet]. 2011;3:436. http://www-pub.iaea.org/MTCD/publications/PDF/p1531interim_web.pdf
- Maharjan S, Parajuli K, Sah S, Poudel U. Knowledge of radiation protection among radiology profes-sionals and students: A medical college-based study. Eur J Radiol Open. 2020 Nov 22;7: 100287. https://doi.org/10.1016/j.ejro.2020.100287
- Eder H, Panzer W, Schöfer H. Ist der Bleigleichwert zur Beurteilung der Schutzwirkung bleifreier Rönt-genschutzkleidung geeignet? [Is the lead-equivalent suited for rating protection pro-perties of lead-free radiation protective clo-thing?]. Rofo. 2005 Mar;177(3):399-404. Ger-man. https://doi.org/10.1055/s-2005-857885
- Bell D, Mann J. Dosimeters. In: Radiopaedia.org [Inter-net]. Radiopaedia.org; 2017. http://radiopaedia.org/articles/57450
- IAEA. Practical Radiation Technical. IAEA-PRTM-1. [Internet]. 2004;(Rev. 1):71.https://www-pub.iaea.org/MTCD/Publications/PDF/PRTM-3r1_web.pdf
- NNRA. Nuclear Safety And Radiation Protection Act (1995 No. 19) Nigerian Transportation of Radioactive Sources Regulations, 2006. [Internet]. 2006;(19):20.
- ICRP. ICRP Publication 103 The 2007 Recommendations of the International Commission on Radiolo-gical Protection. 2007. https://www.icrp.org/publication.asp?id=ICRP+Publication+103
- Okaro AO, Ohagwu CC, Njoku J. Evaluation of Personnel Radiation Monitoring in Radiodiagnostic Centers in South Eastern Nigeria. African J Basic Appl Sci. 2010;2(2):49–53. https://www.academia.edu/87536562/Evaluation_of_Personnel_Radiation_Monitoring_in_Radiodiagnostic_Centres_in_South_Eastern_Nigeria?uc-sb-sw=2749899
- Yusuf SD, Umar I, Bukar I, Idris MM. Assessment of the Knowledge and Attitude to Radiation Safety Standards of the Radiological Staff in Damaturu, Yobe State, Nigeria. 2020;3(3):1–7. https://www.researchgate.net/publication/348560215_Assessment_of_the_Knowledge_and_Attitude_to_Radiation_Safety_Standards_of_the_Radiological_Staff_in_Damaturu_Yobe_State_Nigeria
- Skam JD, Gloria II, Ibrahim ZY, Joseph Zira D. Radiographic Room Design and Layout for Radiation Protection in Some Radio-Diagnostic Facilities in Katsina State, Nigeria. J ARN. 2017;31(1):23. https://www.researchgate.net/publication/320538824_Radiographic_Room_Design_and_Layout_for_Radiation_Protection_in_Some_Radio-Diagnostic_Facilities_in_Katsina_State_Nigeria
- Maina PM, Motto JA, Hazell LJ. Investigation of radiation protection and safety measures in Rwandan public hospitals: Readiness for the implemen-tation of the new regulations. J Med Imaging Radiat Sci [Internet]. 2020;51(4):629–38. https://doi.org/10.1016/j.jmir.2020.07.056
- MCO, Anakwue AM. Radiation exposure from diagnostic radiography: an assessment of X-ray beam collimation practice in some Nigerian Hospi-tals. Internet J Med Update. 2010;5(2):31–3. https://scispace.com/pdf/radiation-exposure-from-diagnostic-radiography-an-assessment-3iv0nwfjx9.pdf?
- Arabia S, Al-sayyari AA, Kalagi S. Assessment of Radiation Protection practices among Univer-sity Students, Buraydah, Saudi Arabia. [Inter-net]. 2021; https://www.iosrjournals.org/iosr-jdms/papers/Vol17-issue3/Version-5/N1703057177.pdf?
- Fiagbedzi E, Gorleku PN, Nyarko S, Asare A, Ndede GA.
Assessment of radiation protection knowledge and practices among radiographers in the central region of Ghana. Radiat Med Prot [In-ternet]. 2022;3(3):146–51. https://doi.org/10.1016/j.radmp.2022.06.001 - Lewis S, Downing C, Hayre CM. Radiography South African radiographers’ radiation protection practices, a qualitative study. Radiography [In-ternet]. 2022;28(2):387–93. https://doi.org/10.1016/j.radi.2021.12.008
Appendix
Table 3.2: ASSESSMENT OF RADIOGRAPHER’S PERCEPTION ON THE INTEGRITY OF THE X-RAY ROOM SHIELDING
Variables
SD (%)
D
(%)
N
(%)
A
(%)
SA
(%)
Mean±S.D
Remark
The X-ray rooms design are purpose-built for radiological procedures
00(0.0)
03(4.2)
03(4.2)
12(16.7)
54(75.0)
4.63±0.76
Strongly agree
The lead-lined walls and doors in the X-ray room are in good condition
00(0.0)
07(9.7)
08(11.1)
24(33.3)
33(45.8)
4.15±0.97
Agree
The X-ray control room is adequately shielded to reduce radiation exposure to the operator
00(0.0)
09(12.5)
04(5.6)
21(29.2)
38(52.8)
4.22±1.02
Strongly agree
The availability of radiation shielding equipment (lead aprons, lead gloves, googles, gonad shields, and thyroid shields) are adequate
01(1.4)
15(20.8)
03(4.2)
35(48.6)
18(25.0)
3.75±1.10
Agree
The shielding devices (lead aprons, lead gloves, googles, gonad, and thyroid shields) are in good condition
00(0.0)
09(12.5)
14(19.4)
34(47.2)
15(20.8)
3.76±0.93
Agree
The personnel dosimeter for radiographers are adequate and in good condition
10(13.9)
21(29.2)
04(5.6)
25(34.7)
12(16.7)
3.11± 1.37
Neutral
The calibration of the X-ray machine is accurate
02(2.8)
11(15.3)
15(20.8)
30(41.7)
14(19.4)
3.60±1.06
Agree
The X-ray machine is equipped with appropriate safety interlocks to prevent accidental exposure.
02(2.8)
07(9.7)
14(19.4)
29(40.3)
20(27.8)
3.81±1.04
Agree
The distance between the X-ray tube and the erect bucky is 180 cm from the focal spot
05(6.9)
07(9.7)
13(18.1)
26(36.1)
21(29.2)
3.71±1.19
Agree
QUESTIONNAIRE
Department of Medical Radiography and Radiological Sciences,
Faculty of Health Sciences and Technology
College of Medicine,
University of Nigeria, Enugu Campus,
August, 2023
Dear Respondent,
This research questionnaire assessed standard radiation protection practices in the radiography departments of several selected tertiary hospitals in southeastern Nigeria.
This research was carried out by the Authors. This study is being conducted for academic purposes, and the researchers will be grateful if you provide answers to the questions posed with the utmost sincerity.
Please note that the strictest confidentiality will be assured with respect to the response given as facts are needed for academic purposes.
Thank you for your anticipated cooperation.
Yours faithfully,
Authors
SECTION A: SOCIO-DEMOGRAPHIC DATA
Instruction: Kindly tick [√] against the option of your choice.
- Gender: a) Male [ ] b) Female [ ]
- Age: a) 21-35 [ ] b) 36-50 [ ] c)51 and above [ ]
- Rank: a) Intern/Corps member [ ] b) Basic radiographer [ ] c) Senior/Principal radiographer [ ] d) Asst Chief/Chief radiographer [ ]
- Years of practice: a) 1-5 [ ] b) 6-10 [ ] c) 11-15 [ ] d) 16-20 [ ] e) 21 and above [ ]
- Highest Qualification: a) B.Sc. [ ] b) M.Sc. [ ] c) Ph.D. [ ] d) Others specify [ ]
- Hospital of practice
- UNTH [ ] b) NOHE [ ]
c) FMC Abakaliki [ ] d) NAUTH [ ]
SECTION B: ASSESSMENT OF THE INTEGRITY OF THE SHIELDING EQUIPMENT USED AND THE X-RAY ROOM DESIGN IN REDUCING RADIATION EXPOSURE IN SOME SELECTED TERTIARY HOSPITALS IN SOUTH EASTERN NIGERIA.
Please tick (√) in the appropriate box
Strongly Agree (SA), Agree (A), Disagree (D), Strongly Disagree (SD), and Not Sure (NS).
SECTION C: EVALUATION OF THE LEVEL OF RADIATION PROTECTION KNOWLEDGE—AND ITS APPLICATION—EXHIBITED BY RADIOGRAPHERS IN SOME-SELECTED TERTIARY HOSPITALS IN SOUTH EASTERN NIGERIA.
Please tick (√) in the appropriate box
Strongly Agree (SA), Agree (A), Disagree (D), Strongly Disagree (SD), and Not Sure (NS).
S/N
Measures to reduce the incidence of medical litigation among practicing radiographers
SA
A
D
SD
NS
1.
I understand the principles of radiation protection and the regulatory guidelines and local protocols related to radiation safety.
2.
I am aware of the appropriate safety measures to minimize radiation exposure to patients and staff
3.
I am aware of the proper use and maintenance of radiation shielding devices and equipment
4,.
The healthcare workers in my hospital received formal training inradiation safety and protection
5.
I consistently apply radiation safety practices during radiographic procedures.
6.
I encourage patients to follow radiation safety guidelines during their examinations
7.
I ensure that patients wear appropriate protective devices during radiographic procedures.
8.
As a radiographer, I keep myself updated with the latest advancements in radiation protection practices.
SECTION D: ASSESSMENT OF THE EFFECTIVENESS OF WORKPLACE AND PERSONNEL MONITORING AND QUALITY CONTROL IN SOME-SELECTED TERTIARY HOSPITALS IN SOUTH EASTERN NIGERIA.
Please tick (√) in the appropriate box
Strongly Agree (SA), Agree (A), Disagree (D), Strongly Disagree (SD), and Not Sure (NS).
S/N
Assessment of the effectiveness of workplace and personnel monitoring and quality control in some selected tertiary hospitals in south eastern Nigeria
SA
A
D
SD
NS
1.
There is a well-defined established radiation safety protocols and quality assurance procedures in your hospital
2.
The established workplace protocol are consistently implemented and followed
3.
The X-ray rooms are often assessed for structural integrity and radiation leakage
4.
The radiation shielding equipment are regularly assessed for structural integrity and radiation leakage
5.
There are mechanisms in place to address and rectify equipment malfunctions promptly.
6.
The personnel dosimetry (e.g., badges) are provided to healthcare workers regularly exposed to radiation
7.
The personnel dosimeters are frequently exchanged and analyzed for radiation exposure
8.
There is a mechanism in place to raise awareness among healthcare workers about the importance of radiation safety
References
Madsen MT, Anderson JA, Halama JR, Kleck J, Simpkin DJ, Votaw JR, et al. AAPM Task Group 108: PET and PET/CT Shielding Requirements. Med Phys [Internet]. 2005 Dec 19;33(1):4–15. http://doi.wiley.com/10.1118/1.2135911
Abdelrahman MA, Abu Alfwares A, Alewaidat H, Alhasan M, Rawashdeh MA, Al Mousa DS. Compliance With Radiation Protection Practices Among Radiologists. Health Phys [Internet]. 2018 Sep;115(3):338–343. https://doi.org/10.1097/hp.0000000000000886
Eze C, Irurhe N, Njoku J, Olowu O, Abonyi L. Assessment of radiation protection practices among radiographers in Lagos, Nigeria. Niger Med J [Internet]. 2013;54(6):386. https://doi.org/10.4103/0300-1652.126290
IAEA. Justification and optimization | IAEA. [Internet]. 2011. Available from: https://www.iaea.org/resources/rpop/resources/international-safety-standards/justification-and-optimization
Kim JH. Three principles for radiation safety: time, distance, and shielding. Korean J Pain [Internet]. 2018 Jul 31;31(3):145–6. Available from: http://www.epain.org/journal/view.html?doi=10.3344/kjp.2018.31.3.145
ANSTO. What is radiation? [Internet]. 2023. Available from: https://www.ansto.gov.au/education/nuclear-facts/what-is-radiation
Ahern M, McEntee MF, Moore N. Radiographers' attitudes toward the use of lead contact shielding. J Med Imaging Radiat Sci. 2023 Sep;54(3):415–420. https://www.jmirs.org/article/S1939-8654(23)01798-8/fulltext.
Vañó E, Miller CJ, Rehani MM, Kang K, Rosenstein M, Ortiz-López P, et al. Annals of the ICRP [Internet]. Vol. 44, Protection, International Commission on Radiological. 2015. 1–143 p. Available from: www.icrp.org
Cherry SR, Sorenson JA, Phelps ME. Radiation Safety and Health Physics. In: Physics in Nuclear Medicine [Internet]. Elsevier; 2012. p. 427–42. Available from: https://linkinghub.elsevier.com/retrieve/pii/B978141605198500023X
Connor N. What is ALARA. Connor, Nick [Internet]. 2019;1. Available from: https://www.radiation-dosimetry.org/what-is-alara-definition/
NNRA. Nigerian Radiation Safety in Diagnostic and Interventional Radiology Regulations, 2006. [Internet]. 2006;(19):661–92. Available from: https://nnra.gov.ng/nnra/page-diagnostic___interventional_radiology
IAEA. Radiation Protection and Safety of Radiation Sources: International Basic Safety Standards. IAEA Safety Standards Series No. GSR Part 3. [Internet]. 2011;3:436. Available from: http://www-pub.iaea.org/MTCD/publications/PDF/p1531interim_web.pdf
Maharjan S, Parajuli K, Sah S, Poudel U. Knowledge of radiation protection among radiology professionals and students: A medical college-based study. Eur J Radiol Open. 2020 Nov 22;7:100287. https://doi.org/10.1016/j.ejro.2020.100287
Eder H, Panzer W, Schöfer H. Ist der Bleigleichwert zur Beurteilung der Schutzwirkung bleifreier Röntgenschutzkleidung geeignet? [Is the lead-equivalent suited for rating protection properties of lead-free radiation protective clothing?]. Rofo. 2005 Mar;177(3):399-404. German. https://doi.org/10.1055/s-2005-857885
Bell D, Mann J. Dosimeters. In: Radiopaedia.org [Internet]. Radiopaedia.org; 2017. Available from: http://radiopaedia.org/articles/57450
IAEA. Practical Radiation Technical. IAEA-PRTM-1. [Internet]. 2004;(Rev. 1):71. Available from: https://www-pub.iaea.org/MTCD/Publications/PDF/PRTM-3r1_web.pdf
NNRA. Nuclear Safety And Radiation Protection Act (1995 No. 19) Nigerian Transportation of Radioactive Sources Regulations, 2006. [Internet]. 2006;(19):20.
ICRP. ICRP Publication 103 The 2007 Recommendations of the International Commission on Radiological Protection. 2007. https://www.icrp.org/publication.asp?id=ICRP+Publication+103
Okaro AO, Ohagwu CC, Njoku J. Evaluation of Personnel Radiation Monitoring in Radiodiagnostic Centers in South Eastern Nigeria. African J Basic Appl Sci. 2010;2(2):49–53. https://www.academia.edu/87536562/Evaluation_of_Personnel_Radiation_Monitoring_in_Radiodiagnostic_Centres_in_South_Eastern_Nigeria?uc-sb-sw=2749899
Yusuf SD, Umar I, Bukar I, Idris MM. Assessment of the Knowledge and Attitude to Radiation Safety Standards of the Radiological Staff in Damaturu, Yobe State, Nigeria. 2020;3(3):1–7. https://www.researchgate.net/publication/348560215_Assessment_of_the_Knowledge_and_Attitude_to_Radiation_Safety_Standards_of_the_Radiological_Staff_in_Damaturu_Yobe_State_Nigeria
Skam JD, Gloria II, Ibrahim ZY, Joseph Zira D. Radiographic Room Design and Layout for Radiation Protection in Some Radio-Diagnostic Facilities in Katsina State, Nigeria. J ARN. 2017;31(1):23. https://www.researchgate.net/publication/320538824_Radiographic_Room_Design_and_Layout_for_Radiation_Protection_in_Some_Radio-Diagnostic_Facilities_in_Katsina_State_Nigeria
Maina PM, Motto JA, Hazell LJ. Investigation of radiation protection and safety measures in Rwandan public hospitals: Readiness for the implementation of the new regulations. J Med Imaging Radiat Sci [Internet]. 2020;51(4):629–38. Available from: https://doi.org/10.1016/j.jmir.2020.07.056
MCO, Anakwue AM. Radiation exposure from diagnostic radiography: an assessment of X-ray beam collimation practice in some Nigerian Hospitals. Internet J Med Update. 2010;5(2):31–3. https://scispace.com/pdf/radiation-exposure-from-diagnostic-radiography-an-assessment-3iv0nwfjx9.pdf?
Arabia S, Al-sayyari AA, Kalagi S. Assessment of Radiation Protection practices among University Students, Buraydah, Saudi Arabia. [Internet]. 2021; Available from: https://www.iosrjournals.org/iosr-jdms/papers/Vol17-issue3/Version-5/N1703057177.pdf?
Fiagbedzi E, Gorleku PN, Nyarko S, Asare A, Ndede GA. Assessment of radiation protection knowledge and practices among radiographers in the central region of Ghana. Radiat Med Prot [Internet]. 2022;3(3):146–51. Available from: https://doi.org/10.1016/j.radmp.2022.06.001
Lewis S, Downing C, Hayre CM. Radiography South African radiographers’ radiation protection practices, a qualitative study. Radiography [Internet]. 2022;28(2):387–93. https://doi.org/10.1016/j.radi.2021.12.008
Downloads
Published
Data Availability Statement
All data generated or analyzed during this study are available from the corresponding author upon reasonable request. The datasets supporting the conclusions of this article have been securely archived and can be accessed for further assessment, subject to ethical and legal considerations. This work has been published in the Swiss Journal of Radiology and Nuclear Medicine.
Issue
Section
License
Copyright (c) 2025 Ibe, Chijioke K., Ezenwaka, Augusta Amarachi, Ezugwu, Wisdom K., Ifeanyi, Thankgod O., Nwadike, Uchechukwu I.

This work is licensed under a Creative Commons Attribution 4.0 International License.
This license requires that reusers give credit to the creator. It allows reusers to distribute, remix, adapt, and build upon the material in any medium or format, even for commercial purposes.








