Vol. 22 No. 1 (2025): Vol. 22 No. 1 (2025)
Original Research:
Transient Headache as a Complication of Bronchial Artery Embolization for Hemoptysis
https://doi.org/10.59667/sjoranm.v22i1.16
Background: Bronchial artery embolization (BAE) is an established treatment for hemoptysis. While major complications are well documented, transient headaches during the procedure are rarely reported.
Purpose: To determine the frequency, characteristics, and potential mechanisms of headaches occurring during BAE.
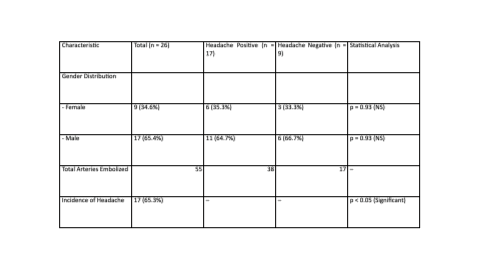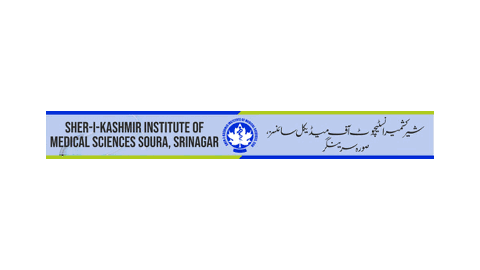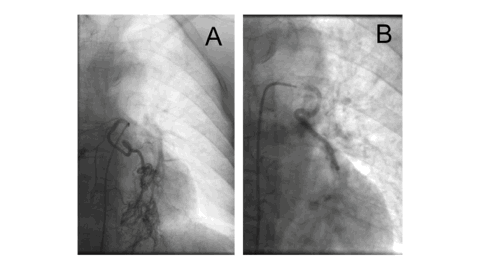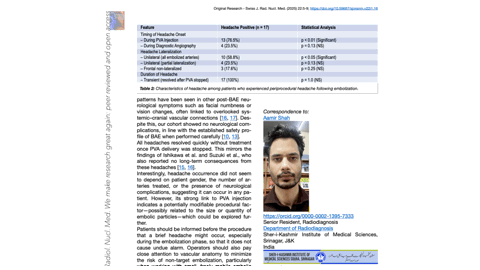
Methods: Twenty-six patients (17 male, 9 female; mean age 62.3 ± 13.5 years) undergoing BAE for hemoptysis were prospectively evaluated. All procedures were performed under conscious sedation, using superselective catheterization and polyvinyl alcohol (PVA) particles. Headache onset, duration, location, and relation to procedural stage were recorded. Neurological examination was performed immediately post-procedure. Statistical analysis used Fisher’s exact test.
Results: Headache occurred in 17 patients (65.3%). Most episodes arose during PVA injection (76.5%, p < 0.01) and were unilateral in 58.8%, corresponding to the treated side (p < 0.05). All headaches resolved spontaneously after embolization stopped. No patient required analgesics, and no neurological deficits were detected. Headache incidence was unrelated to gender, number of arteries embolized, or underlying cause of hemoptysis.
Conclusion: Transient headache is a relatively frequent and benign event during BAE, often associated with PVA injection and lateralizing to the embolized side. Awareness of this phenomenon allows better patient counselling and procedural reassurance.
Case Report:
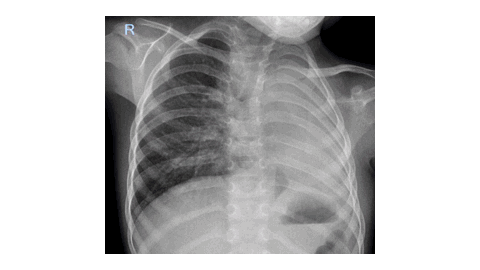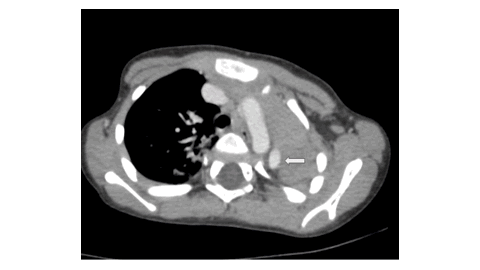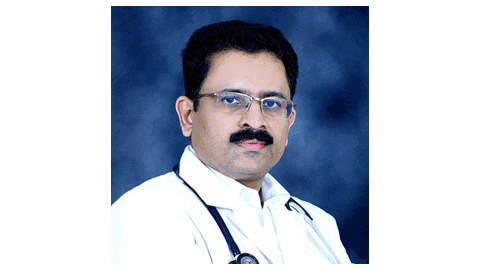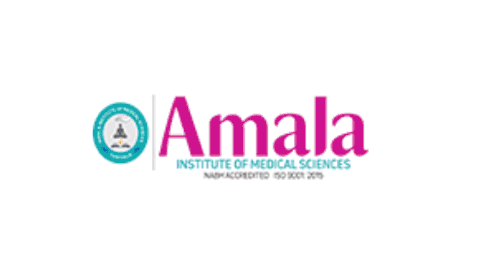
The Unilateral Pulmonary Aplasia: Radiologic Clues to a Congenital Anomaly
https://doi.org/10.59667/sjoranm.v22i1.14
Pulmonary aplasia is a rare congenital developmental malformation characterized by total absence of lung with rudimentary bronchus. Although the exact cause is not known, several factors have been proposed. Patients can be asymptomatic or can present with recurrent respiratory infections. Multimodality imaging may be needed for confirmation and needs to be differentiated from pulmonary agenesis or severe hypoplasia. This case highlights the key imaging findings of pulmonary aplasia and the need for early diagnosis so as to prevent further complications.
Case Report:
Ciliated Hepatic Foregut Cyst: A Case-Report and Literature Review
https://doi.org/10.59667/sjoranm.v22i1.18
The ciliated hepatic foregut cyst (CHFC) is a rare benign cystic lesion of the liver. Since its initial description fewer than one hundred cases have been reported in the literature. CHFCs are usually asymptomatic and often discovered incidentally during imaging for other reasons. They are most often located in the anterior subcapsular region of segment IV of the liver. The definitive diagnosis is histopathological.
CASE REPORT
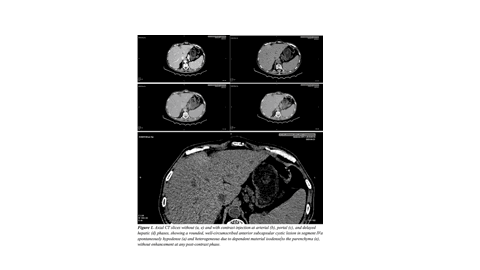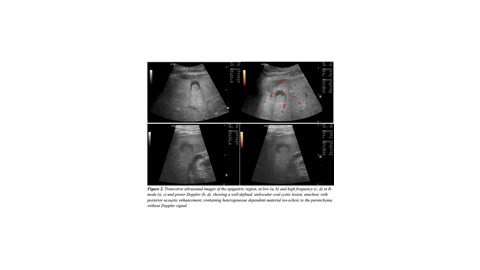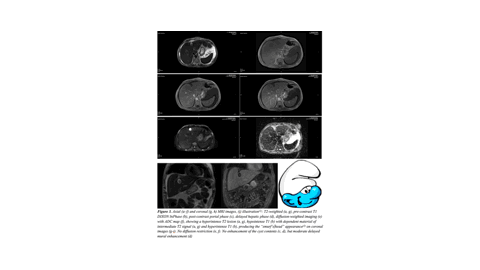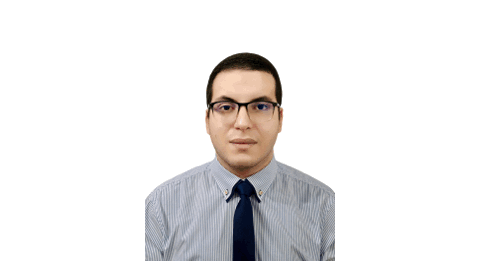
We report the case of a 60-year-old man with no significant medical or surgical history who underwent a thoraco-abdomino-pelvic CT scan as part of the workup for a pathological fracture of the left femur. It revealed an oval, well-circumscribed cystic lesion in the anterior subcapsular region of segment IVa. US and MRI were used for further assessment.
DISCUSSION
CHFCs are rare cystic liver lesions resulting from abnormal embryonic development. Although benign, rare cases of malignant transformation have been reported . They typically occur in adults between 50 and 55 years, and a slight male predominance. Most cases are asymptomatic. They are characteristically located in the anterior subcapsular region of segment IV —a key diagnostic clue. Ultrasound, is usually the first-line modality. It reveals a well-defined unilocular cyst with dependent echogenic sediment. CT typically shows a spontaneously hypodense lesion without post-contrast enhancement. MRI is the gold standard for lesion characterization. It reveals the pathognomonic “smurf’s head” appearance, as seen in our case. Histological confirmation is recommended. Management remains controversial as CHFC is not purely benign due to its malignant transformation potential.
CONCLUSION
CHFC is a rare benign liver lesion that should be considered in any middle-aged adult presenting with a unilocular cystic lesion in segment IV.